Let's talk about your pain.
>> Do you have constant abdominal pain? Intermittent pelvic pain? Occasional cramps? Cramps that leave you stuck on your couch hugging a heating pad? Sharp shooting pain? Dull stabby pain? Achey drive-you-nuts pain?
| Research shows that osteopathy can | ||||
| significantly reduce pain & dysfunction | ||||
| in many common gynecological | ||||
| conditions such as: | ||||
| - endometriosis | ||||
| - dysmenorrhea (painful periods) | ||||
| - polycystic ovarian syndrome (PCOS) | ||||
| - uterine fibroids | ||||
| - adenomyosis | ||||
| - surgical scarring | ||||
| - pregnancy-related pain | ||||
| - diastasis recti | ||||
| - symphysis pubis | ||||
| - ovarian cysts | ||||
| - adhesions due to complications from | ||||
| ectopic pregnancies | ||||
| - C-section scars | ||||
| - adhesions from hysterectomy, | ||||
| oopherectomy and salpingectomy | ||||
>> Do you think about your pain more often than you feel you should?
>> Do your cramps ever get in the way of you living your life?
>> Do you have a love/hate relationship with your uterus and ovaries?
>> Are you preparing for a pregnancy, currently pregnant, or struggling to recover physically after a pregnancy?
If you have pelvic or abdominal pain, you’re not alone. Your pain is real. One of every seven women is affected by pelvic pain. Research shows that osteopathy can be helpful in reducing pain and improving function for many causes of pelvic pain. Your health is important, it’s worth getting assessed.
Manual therapy (osteopathic visceral manipulation) treatment for pelvic pain.
Osteopathy is often overlooked as a treatment option for the many painful health issues women endure. Beyond medication and surgery, most women aren't aware of the benefits of manual therapy for this kind of pain. Osteopathy is a form of manual therapy that uses gentle, hands-on techniques in a comfortable setting with an aim of reducing the pain and dysfunction caused by pelvic pain. The techniques used are called osteopathic visceral manipulation and clinical research shows that it often helps reduce pain and improves quality of life for women with painful conditions of the pelvis and abdomen. Our clinic provides evidence-based, effective osteopathic care that is based upon your specific symptoms in concert with the care provided by family physicians, gynecologists and other specialists.
Ottawa Osteopathy & Sports Therapy is a teaching clinic for physicians, family doctors, nurse practitioners and sport medicine fellows.
Clinical examination of the pelvis for chronic pelvic pain was presented by our staff at the University of Ottawa, Faculty of Medicine, during a Faculty Development Workshop entitled "Hands-On Special Testing for Differential Diagnosis and Case Management". We also regularly host physician and nurse practitioner seminars on the physical assessment of the lower back and hips. During this seminar, we discuss the importance of screening for and assessing treatable adhesions in the pelvis, which are related to chronic pelvic pain. Assessing and treating chronic pelvic pain with manual therapy has also been presented by our staff at Sport Medicine Rounds, hosted by Carleton University Sport Medicine Clinic.
Our clinic is an observation/preceptor site for both physiotherapy and osteopathy for the University of Ottawa's Sport and Exercise Medicine Program. Sport Medicine Fellows use clinical observation, with our staff, as part of their learning objectives to familiarize themselves with the scope of practice used in these professions.
Want to read research on how effective osteopathic visceral manipulation is for different conditions?
Feel free to click the following links to read recent research on the effectiveness of osteopathic visceral manipulation in treating: endometriosis, deep infiltrating endometriosis with colorectal involvement, dysmenorrhea (painful periods), polycystic ovarian syndrome (ovarian cysts), uterine fibroids, adenomyosis, surgical scarring, pregnancy-related pain, and C-section scars. Osteopathic manual practitioners also offer treatments designed to improve constipation, IBS, symphysis pubis dysfunction, post-surgical adhesions from ectopic pregnancies, post-operative scars related to hysterectomy, oophorectomy, salpingectomy, appendectomy, and other related conditions. There is a growing body of research supporting this non-pharmacological form of care.
What is the treatment? What happens in the appointment?
The appointment will begin with a discussion about your symptoms, your current diagnosis, the treatment plan you are following, your overall health history and the guidance from your family physician, gynecologist or obstetrician. The practitioner will make note of when your symptoms started, what makes them worse, what positions, or activities make them better, what you've tried to do to make them go away, a history of medications (if any), prior treatments and any surgeries. After completing a detailed history, your therapist will perform a physical assessment. This will include looking at how your lower back, hips and other joints of your body move.
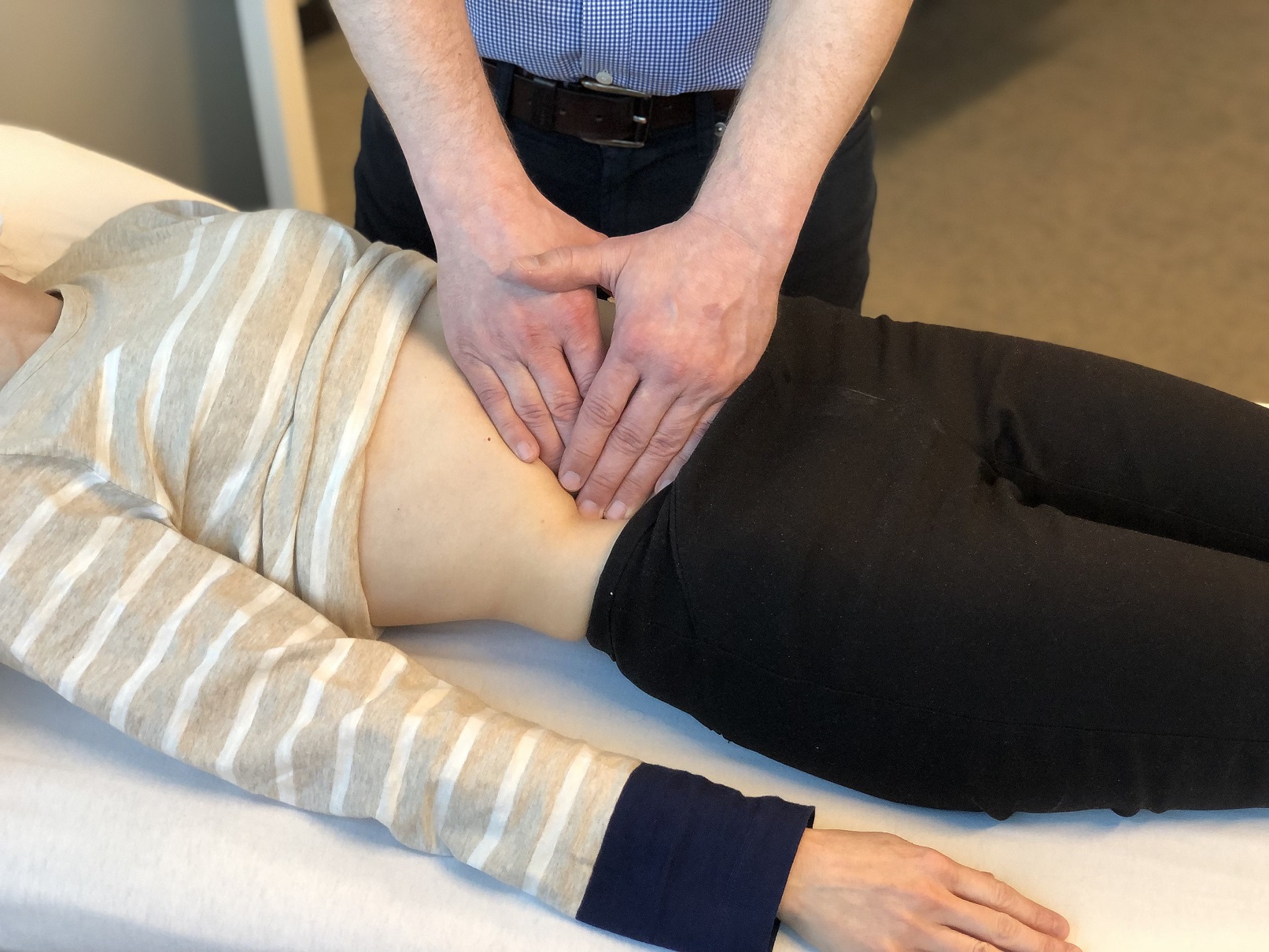 This physical assessment will also include a comprehensive manual palpation of your abdomen, and pelvis using gentle hand pressures.The therapist will note any related tensions, soreness and feel for areas of adhesions. They will record the specific location, density and direction of these restictions and any symptoms produced by the areas assessed. Adhesions are scar-like tissues which make anatomical neighbours stick together. Qualified osteopathic manual practitioners receive extensive professional training with clinical supervision, learning to feel for these adhesions. This specific palpation allows them to perform gentle manual therapy techniques, which research shows can help reduce the tension and symptoms related to these adherent tissues caused by conditions like endometriosis, PCOS, dysmenorrhea and others.
This physical assessment will also include a comprehensive manual palpation of your abdomen, and pelvis using gentle hand pressures.The therapist will note any related tensions, soreness and feel for areas of adhesions. They will record the specific location, density and direction of these restictions and any symptoms produced by the areas assessed. Adhesions are scar-like tissues which make anatomical neighbours stick together. Qualified osteopathic manual practitioners receive extensive professional training with clinical supervision, learning to feel for these adhesions. This specific palpation allows them to perform gentle manual therapy techniques, which research shows can help reduce the tension and symptoms related to these adherent tissues caused by conditions like endometriosis, PCOS, dysmenorrhea and others.
After the evaluation has been completed, treatment can consist of light or moderate pressures to the areas identified by the assessment. Hand pressures may be static and held for 1-3 minutes or there may be gentle slow movements. Your feedback is important, and if pain arises, the technique can be modified to make it more tolerable for you. We regularly check in with you to make sure the treatment is tolerable.
Osteopathic manual practitioners are not medical physicians.
It's important to remember that osteopathic manual practitioners are not medical doctors and do not diagnose. We are manual therapists who work in tandem with your family doctor, gynecologist or medical specialist to provide treatment options aimed at reducing pain and improving quality of life. All new and unusual pains which do not have a clear diagnosis should be assessed by a licensed medical physician. Gynecologists play a key role in the proper diagnosis of the underlying condition, ordering imaging if needed and providing the range of available treatment options. Even complex conditions like endometriosis can now be identified with the help of specific ultrasound imaging when the sonographer has advanced forms of training for this condition. Symptoms which are red flags will be referred back to your primary care physician for proper assessment. If you do not have a family physician or medical specialist following you, you can still be assessed by an osteopathic manual practitioner and if appropriate receive osteopathic care while waiting for a specialist referral.
 Treatment for pregnancy
Treatment for pregnancy
Osteopathy can help women during their pregnancy by improving mobility, function, and decreasing pain and soreness during the 2nd and 3rd trimester. This form of treatment can help with symphysis pubis dysfunction, sciatica, and can help prepare the body for birth. After birth, many women choose to follow up in osteopathy to deal with the aches and pains involved with caring for and carrying an infant, and the physical stresses associated with breastfeeding.
Can I get assessed and treated in osteopathy without a doctor's referral?
Yes. You can book your assessment and treatment without a doctor's referral. If you have a physician guiding your care, we can work with them to coordinate your care. Note that some insurance companies require a referral for forms of care such as physiotherapy and osteopathy for reimbursement.
My pelvic/abdominal pain is different. It's kind of unique. Should I try osteopathy?
Some pelvic pains are sharp and stabbing while other pains can be dull, or achey. It may feel like no one really understands your pain. It is still worth exploring all options to improve your pain. Many of these pains can be assessed, correlated to your clinical physical exam and treated with specific manual therapy in osteopathy. If your pain is bothering you and reducing your quality of life, it's real and it's worth getting assessed.
I'm also experiencing persistent pain in my hip/back/knee - can you treat that too?
Yes. Adhesions and tension in the connective tissues of your abdomen and pelvis can significantly influence pain elsewhere in your body. This means that pain in your lower back, hip, knee, upper back, or even your shoulder may be related to the function of your abdomen and pelvis. A whole body approach of therapy that addresses the sources of these tensions typically results in decreased pain and improved function in both the abdomen and pelvis. This often correlates to an improvement of associated pain elsewhere in your body.  Commonly, patients are under the care of a a gynecologist for pelvic pain, a physiotherapist for hip pain, and a family physician for headaches. Osteopathy addresses the common link in these areas together using a whole body manual therapy approach. This may done be by addressing scar tissue, improving joint mobility or other elements identified by the clinical exam.
Commonly, patients are under the care of a a gynecologist for pelvic pain, a physiotherapist for hip pain, and a family physician for headaches. Osteopathy addresses the common link in these areas together using a whole body manual therapy approach. This may done be by addressing scar tissue, improving joint mobility or other elements identified by the clinical exam.
What if I need or have already had surgery?
Many of our patients have already had multiple surgeries and find that osteopathic visceral manipulation helps reduce the restrictions and adhesions caused by surgery itself. In cases of PCOS, uterine fibroids and endometriosis, your doctor may suggest surgery as an option to excise or remove the cause of the pain. Patients often seek out osteopathic care to reduce pain and improve quality of life while waiting for an appropriate specialist or a surgical intervention. We always follow the post-operative guidance identified by recent research and your surgeon's treatment plan. Surgical adhesions often improve with osteopathic visceral manipulation even when the surgery was performed many years prior.
How many appointments do I need?
There are many causes of pelvic pain and ideally, they should be properly diagnosed by a medical physician. Different people and conditions can respond differently to therapy. Most people see improvement in pain and quality of life after 2-4 treatments, while some more complex cases may need more treatment. Some of the more complex conditions/cases may not respond at all. If we do not feel your symptoms would be improved by osteopathic care, this will be discussed with you and referral suggestions will be offered.
Our osteopathic manual practitioners meet or exceed the World Health organization's benchmarks in osteopathic training.
This benchmark ensures that you are receiving the highest level of osteopathic care available.
Osteopathy services are covered under most extended health care insurnace plans.
We offer direct billing to most insurance companies. It is important to always verify your specific insurance policy's annual limits, inclusions and exclusion details.
Why hasn’t my doctor mentioned this?
Education programs for physicians (example: the University of Ottawa’s School of Medicine) are just beginning to include information on complementary therapies such as osteopathy. Unless your physician, gynecologist or specialist has personally sought out to learn about osteopathic care, it is unlikely they received information about it during their formal education. Evidence-based complementary therapies such as osteopathy strive to work with your primary care physician to provide additonal forms of therapy aimed at reducing pain and improving quality of life. If your doctor has questions about this form of therapy, we’d be happy to speak with them to form a greater continuum of care.
What if I am also experiencing pelvic floor dysfunction, anxiety or depression?
Our multi-disciplinary team of caring practitioners is connected to many other specialized health care providers in the city. We can connect you to other professionals such as a pelvic floor physiotherapist or a psychologist.
Watch Women's Health: Finding Relief through Osteopathy to learn more about recent research and case studies from treatment.
Want to learn more about the research that supports this treatment approach? Hear about actual treatment outcomes from women with these conditions? Watch our the video we created on Women's Health: Finding Relief through Osteopathy.
Book your first appointment:
If you want to get started with treatment , please click here to book online. You can also email us at . or call us at (613) 521-3222. We're here to help.






